Room 1: Introduction
- Introduction
- Epileptic Seizures
- Types of epilepsies
- Causes of epilepsy
- Treatment
- Acute and emergency therapy
- Long-term therapy - Consequences
What is Epilepsy?
Introduction
Hardly any other illness can be traced back in medical history as far as epilepsy can. Many pointers from early history indicate that this condition has been part of the human lot from the very beginning. Then as now, it is
one of the most common chronic diseases that there are: 0.5% of all human beings suffer from epilepsy, which means that in the U.K. alone around 300 000 to 600 000 people are affected.
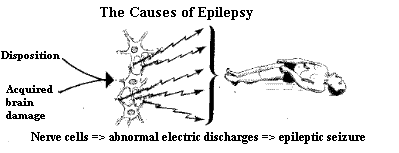 How can epilepsy be defined? When someone repeatedly has epileptic seizures then we say that that person is suffering from epilepsy. An epileptic seizure itself is one of the many pathological forms of reaction which can take place in the brain; it is the brains "response" or reaction to a disturbing, irritating or damaging stimulus. This reaction to the stimulus is accompanied by abnormal electro-chemical excitatory processes in the cerebral nerve cells. This pathological process takes place when suddenly an unnaturally large number of nerve cells are stimulated simultaneously, causing a difference in voltage between the outer side of the cell wall and the inside of the cell (membrane potential). This voltage difference is then suddenly discharged, creating a kind of "storm in the brain", or, to put it another way, "making a fuse blow".
How can epilepsy be defined? When someone repeatedly has epileptic seizures then we say that that person is suffering from epilepsy. An epileptic seizure itself is one of the many pathological forms of reaction which can take place in the brain; it is the brains "response" or reaction to a disturbing, irritating or damaging stimulus. This reaction to the stimulus is accompanied by abnormal electro-chemical excitatory processes in the cerebral nerve cells. This pathological process takes place when suddenly an unnaturally large number of nerve cells are stimulated simultaneously, causing a difference in voltage between the outer side of the cell wall and the inside of the cell (membrane potential). This voltage difference is then suddenly discharged, creating a kind of "storm in the brain", or, to put it another way, "making a fuse blow".
If a person has one epileptic fit, it does not mean that he or she has epilepsy. Only when that person suffers repeated spontaneous epileptic seizures (i.e. without any direct trigger), should they be diagnosed as having epilepsy. Epilepsy is therefore always a chronic illness which can go on for many years (but which does not necessarily last a lifetime!).
The term "epilepsy" is derived from the Greek word "epilambanein", which means "to seize upon", "to attack". Thus epilepsy is a seizure or rather a disease which causes seizures to occur. As, however, there are many very different types of seizure, it is better to speak of epilepsies.
Epileptic Seizures
Epileptic seizures can look very different. There is hardly any function of the brain which cannot also be part of an epileptic seizure. As a result, seizures can manifest themselves in many different ways: in movements (e.g. jerking, trembling, stiffening of the muscles), in paralgiae/ sensory disturbances (e.g. tingling, numbness, hearing or seeing something), in so-called vegetative signs (e.g. flushing, lips turning blue, salivation, bowel sounds, wetting oneself), or in psychological changes (e.g. fear, sudden memory impairment, loss of consciousness).
These manifestations often occur in combination, for instance stiffening, jerking, salivation, wetting oneself and loss of consciousness are symptoms of a "major seizure", a "grand mal" ("great evil"). In the past, people differentiated between such "major" seizures and "lesser", "petit mal" attacks, which manifest themselves in a short clouding of the consciousness or absence) which only lasts for a few seconds, in a single jerk (myoclonia) or in a so-called twilight state. These seizures, which are also termed psycho-motor or partial complex seizures, are characterised by a twilight state lasting between 30 seconds and 3 minutes, during which the patient is confused, displays inappropriate behaviour (e.g. chewing movements, fiddling with the hands, running away) and sometimes utters intelligible but meaningless words, or incomprehensible sounds. The salaam spasm is a special form of petit mal seizure which occurs almost exclusively in infants and which is generally a pointer for a severe type of epilepsy. (The "salaam seizure" is so called because of the nature of the seizure, during which the patient suddenly jerks, nods or slowly bends forward, as if to make an oriental greeting.)
Today specialists no longer speak of "grand mal" and "petit mal" seizures, but "generalised" and "focal" seizures.
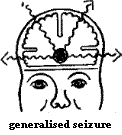 During a generalised seizure, both halves of the brain are affected simultaneously and thus the attack influences both sides of the body from the onset. This does not necessarily mean that the whole body is affected by the seizure; what is primarily important is the simultaneous nature of the attack from the onset.
During a generalised seizure, both halves of the brain are affected simultaneously and thus the attack influences both sides of the body from the onset. This does not necessarily mean that the whole body is affected by the seizure; what is primarily important is the simultaneous nature of the attack from the onset.
 The above-mentioned grand mal seizures, absences and salaam seizures are all generalised seizures.
The above-mentioned grand mal seizures, absences and salaam seizures are all generalised seizures.
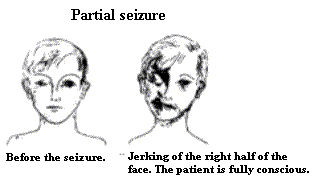
Focal seizures are in contrast attacks which at the onset only affect one side of the body or a certain part of the body. (This in its turn means that in the brain only a certain part of one hemisphere is affected by the seizure.) Examples of focal seizures are one sided grand-mal seizures, one-sided jerking, stiffening or dysaesthesia, and psychomotor (partial complex) seizures.
Types of Epilepsy
If a person suffers one epileptic seizure, it does not necessarily mean that he or she has epilepsy. Such a seizure can remain a one-off occurrence, e.g. a convulsion during fever in infancy, a seizure caused by an electric shock or by excessive consumption of alcohol and/or lack of sleep after a night of drinking. In such cases, the seizure is linked to a certain situation and provoked by certain circumstances and is therefore known as an occasional convulsion. 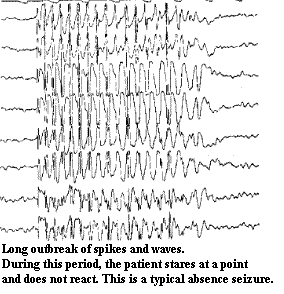 However, as an attack of fever does not trigger an epileptic seizure in every infant, and excessive alcohol consumption does not bring on a convulsion in every adolescent, the person who suffers an attack in such circumstances must also have a certain
tendency or predisposition to epileptic seizures.
However, as an attack of fever does not trigger an epileptic seizure in every infant, and excessive alcohol consumption does not bring on a convulsion in every adolescent, the person who suffers an attack in such circumstances must also have a certain
tendency or predisposition to epileptic seizures.
Only when epileptic seizures occur repeatedly and spontaneously, without any clear trigger, can epilepsy be given as a diagnosis.
There are many very different types of epilepsy. They are primarily characterised by the outward symptoms of the epileptic seizures, but also by the cause, the course of the disease, its prognosis (the probable outcome of the disease) and by the EEG findings (EEG: electroencephalography).
All these factors can vary greatly depending on the type of epilepsy. The types of epilepsy are also differentiated into generalised and focal forms, depending on whether they cause generalised or focal seizures.
Causes
There are many different causes of the various types of epilepsies. Most epilepsies are residual epilepsies, which means that the epilepsies are the "remains" of a cerebral disorder which occurred in the past. Such residual epilepsies can be traced back to in infection of the mother during pregnancy (e.g. rubella), to oxygen deficiency at birth, to encephalitis or meningitis in childhood or to cerebral contusion (brain damage) caused by a traffic accident.
Process epilepsy is a type of epilepsy caused by a progressive cerebral disease which is still active. The most significant and common cause of this type of epilepsy is a brain tumour, but it can also be caused by disturbed blood circulation or metabolic diseases. Epilepsies which are the symptom of a residual or progressive cerebral disorder are called symptomatic epilepsies.
Epilepsies are not hereditary diseases, they cannot be passed on from one generation to the next. Nevertheless there can be a cluster of cases of epilepsy in certain families. This is because - as with many diseases, for instance diabetes or rheumatism - the illness itself is not hereditary, but the
predisposition to it is. Any additional disorder, e.g. complications during pregnancy or at birth, a serious illness or a head injury, can trigger the onset of epilepsy. It is, however, not always possible to find the actual trigger of the disease. Such a type of epilepsy, which is mainly caused by genetic disposition is known as a genetic epilepsy. In around one third of all epilepsies, the cause of the disease remains unknown.
It is clear, therefore, that anyone can get epilepsy at any time in their life.
Treatment
Acute and emergency therapy:
![]() Instructions for the layman
Instructions for the layman
Long-term therapy:
Today, there are very good methods available for treating of epilepsy. Certain types of epilepsy are curable. Before beginning treatment, the patient has to be examined to ascertain whether the cause of the epilepsy can be removed. If this is the case, then a so-called causal therapy can be undertaken, e.g. the removal of a brain tumour, or the curing or alleviation of a metabolic disorder. In most cases, however, this is not possible, either because no cause for the disease can be found, or because it cannot be removed (e.g. a scar in the brain, an anomaly in the brain, or predisposition). The treatment of these types of epilepsies is known as symptomatic therapy.
The "classic" symptomatic therapy, used in over 90% of all cases of epilepsy, is the administration of 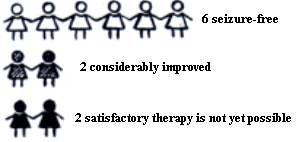 anti-epileptic drugs, which generally have to be taken over several years. Almost 60% of all patients who take these drugs become seizure-free, while the condition of a further 20% is considerably improved.
anti-epileptic drugs, which generally have to be taken over several years. Almost 60% of all patients who take these drugs become seizure-free, while the condition of a further 20% is considerably improved.
In some cases, patients can be successfully treated using epilepsy surgery. However, this is only possible with focal epilepsies and can only be considered as an option in 5% of all patients.
Consequences
Epileptic seizures do not destroy brain cells; therefore the intelligence of an epileptic patient does not necessarily deteriorate during the course of the disease. This is not true of the so-called status epilepticus, however. This state is an unusually long grand mal seizure, which can go on for 10 minutes or more, and even last for hours! During such a state, brain cells can be destroyed. Fortunately such grand mal states occur very rarely today thanks to modern drug therapy.
If epileptic patients have mental abnormalities, e.g. mental retardation, behavioural or speech disorders, these are not usually caused by the epilepsy but by the brain disorder which itself is the cause of the epilepsy. Patients generally tolerate the anti-epileptic drugs well. In exceptional cases, however, the drugs can have serious side-effects and harm the patient. The treatment must therefore be conducted under regular medical supervision by a specialist.
People with epilepsy often suffer from reactive disorders. It is often difficult to come to terms with the disease, and many people experience disadvantages in everyday life: rejection at school, at work and in other social groups (e.g. when doing sport, learning to drive, or applying for a job). The prejudices which many have against people with epilepsy, e.g. the assumption that they have a hereditary or mental disease, often put them under immense psychological stress, which can sometimes be more serious than the epilepsy itself. This is a very important factor in the care of epileptic patients.
 What is Epilepsy?
What is Epilepsy?